Four healthcare professionals who led the initiative to transition from multidisciplinary to interdisciplinary teams within the rehabilitation centre, referred to in this study as change initiators, participated in the focus group. Their gender and discipline of participants could render them identifiable so we have omitted that information from the manuscript. In the focus group, participants were asked to reflect on the interdisciplinary team (IDT) framework and discuss the practical changes they had implemented or proposed within their teams. These changes are outlined in Table 1.
However, participants also identified several barriers to implementing these changes as three resulting themes from the reflexive thematic analysis are presented in this section with 10 sub-themes encompassed (see Fig. 1). These highlight the complexities of embedding interdisciplinary approaches in practice and align with existing research on the difficulties of organisational change in healthcare settings. Each theme illuminates different dimensions of an overall conceptualisation of IDT working as a disruption of the status quo in a rehabilitation healthcare organisation.
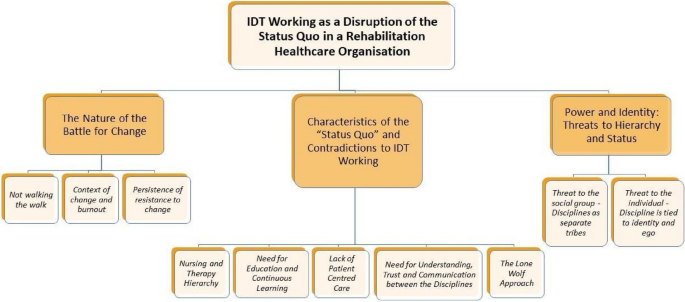
Themes from the reflexive thematic analysis
Theme 1: the nature of the battle for change
Subthemes: Not walking the walk, Context of change and burnout, Persistence of resistance to change.
This theme captures an overall narrative in which creating changes to healthcare teams was conceived of as a battle, with staff often resistant to introduced changes.
Subtheme: not walking the walk
Participants noted a contradiction: while many staff verbally supported IDT principles, they hesitated to address team problems actively. IDT became a label rather than a guiding practice. Participants observed that while people were willing to discuss IDT values “beneath the surface” there was often a lack of motivation to truly embed these values into practice and tackle ongoing team issues. This reluctance is further described in the “persistence of resistance to change” subtheme as a struggle against entrenched attitudes.
Subtheme: context of change and burnout
This sub theme focused on participants’ description of the context in which they were creating changes. It represents participants’ perception of change fatigue within the organization, exacerbated by recent events like COVID-19 and relocation to a new facility. While the pandemic briefly improved teamwork, with a sense of staff pulling together to deal with a crisis, staff burnout and resistance to further change became commonplace. They discussed the specific “non crisis” aspect to a tertiary, non-acute hospital. The comfort of familiarity causing reluctance to change is described by participant 3: “it’s like putting on your comfy clothes, it fits well, I know where I’m going in them”. A sense of busyness and exhaustion seemed to permeate descriptions of staff resistance to change for example: “People are pulled in so many different directions… and then I think that then fed in with COVID and whatever as well. There was a… Everybody was just burnt out. We can’t do anything different anymore… That was the mantra that was common as well… Well, there was a sense of you’re really hardnosed, you’re trying to push through or, you know, kind of continue to change things. Can you not see?” Participant 4.
Theme 1 focuses on participants’ struggle to change the status quo in rehabilitation teams and give a voice to often unspoken issues. Despite surface-level agreement with IDT values, resistance to change and default to the status quo persisted. The subsequent theme explores the characteristics of this status quo and its challenges to IDT implementation.
Subtheme: persistence of resistance to change
This sub-theme captures how, in creating a narrative of their experiences in introducing changes to teams, participants cast themselves as disruptors within a resistant system. They expressed their own “naivety” and their underestimations of how persistently resistant to change the organisation could be. As reflected by participant 2 “I think we all underestimated. I think we all optimistically hoped that people would want to work differently because it would be more satisfying..”
When physical changes to the hospital environment were made with separate siloed departments eradicated in favour or shared IDT spaces—people reconstructed single discipline spaces. In this way aspects of the working culture outlived the physical environment. The participants discovered the discomfort creating changes to teams can cause, and suggested this was because they were endeavouring to speak the unspoken—giving a voice to issues often left unexpressed, raising issues that many did not particularly want to face. To the authors’ interpretation, this created a sense of a ‘battle’ for the participants, illustrated by a latent weariness in their accounts. As participant 3 expressed: “In the same way as the patient forum has done that for years and years and years, but we kind of keep saying it and we also keep adding, so…”.
Theme 2: characteristics of the “status quo” and contradictions to IDT working
Subthemes: Nursing and Therapy Hierarchy, Need for Education and Continuous Learning, Lack of Person Centred Care, Need for Understanding, Trust and Communication between the Disciplines, The Lone Wolf Approach.
The previous theme characterises changes to teamwork as a disruption of the status quo and a battle for the participants, describing the nature of this battle. This theme focuses on the status quo itself and specifically the elements of this that act as obstacles and/or major contradictions to a policy (and underlying values) of IDT working.
Subtheme: nursing and therapy hierarchy
Participants identified a starting point in their work: a divide between nursing staff and therapists. Change initiators described that, in their experience, nursing staff and healthcare assistants often felt undervalued and disconnected from their teams, citing a perceived lack of recognition for their contributions. One example they shared was the reliance on therapists to facilitate breaks for nursing staff, an expectation that therapists were often unaware of, which led to frustration and a sense of being overlooked. This dynamic underscores broader communication and role clarity challenges within the interdisciplinary team. This highlighted not just communication gaps, but also a lack of psychological safety and hierarchical dynamics. Such instances reflected a damaging divide, where frontline staff felt least appreciated. This division was evident in language use, where “the IDT” often referred only to therapists, underscoring the need for education and continuous learning to address misconceptions about IDT working.
Subtheme: need for education and continuous learning
In discussing key aspects of IDT working, particularly emphasizing reflexivity—pausing, reflecting, and learning to adapt—participants highlighted the challenge of translating theoretical knowledge about person-centredness or IDT working into practical application. They created contradictory narratives—while some learn valuable principles during training, some can lose them in entering work environments at odds with that ethos. This sub-theme also represents common misconceptions about teamwork and who constitutes the IDT discussing how, “teamwork is more than people with the same coloured trousers working together” (Participant 2) and how teamwork is more than staff “getting along”. The central idea revolves around the necessity for continuous education and adaptation, with participants emphasizing the importance of learning from others and developing a shared understanding of interdisciplinary teams and rehabilitation. A lack of continuous learning is further reflected in Theme 3 (power and identity) as participants emphasised how one’s professional identity can impede asking questions particularly to other disciplines. This highlights a perceived need for a cultural shift where learning and inquiry are valued.
Subtheme: need for understanding, trust and communication between the disciplines
Participants noted that staff members from different disciplines felt disconnected from each other, both professionally and personally. They discussed activities aimed at fostering understanding of each other’s roles as a crucial step toward building a unified team. They also described get-to-know-each-other activities as humanizing and essential for cultivating empathy and respect among team members. Conflicts between staff were identified as a starting point for their work, with instances sometimes escalating to HR. Participants also noted a culture of unhealthy conflict avoidance, where staff struggled to openly disagree or communicate effectively, hindered by jargon and disciplinary language barriers. Together these codes convey teams with a lack of psychological safety and a culture where different staff of different disciplines can feel threatened by one another (see also “Power and Identity” theme), do not like to disagree and struggle to feel understood and to communicate to other disciplines. The participants tied this culture to many incidents of poor communication and collaboration between team members in practice.
Subtheme: lack of person-centred care
Participants highlighted various discrepancies in core values regarding person-centredness within the organization. Sometimes these were explicit statements made to them “we’re too patient centred now”. They recounted incidents where staff disregarded patient communication or made care decisions lacking in person-centredness. They stressed that person-centred care is crucial to IDT working, emphasizing that issues in teamwork and communication directly impact patient care.
“Talking over patients, yeah, was a big one, you know? Doing… a procedure and talking to the person working with you and not including the patient and even hardly acknowledging them“. Participant 3.
Subtheme: the lone wolf approach
The participants reflected on various incidents and attitudes encountered over recent years and constructed a narrative of individual choice trumping collective responsibility, as Participant 2 outlines:
“So, that sense of collaborative working… It seemed that if you didn’t feel it as an individual, you didn’t have to do it because the team wanted it or needed it or it was part of being a team, you as an individual could just decide to do something different. “ Participant 2 and “There’s a whole lot of stuff like that where it’s the way people have always done it” Participant 1.
Participants emphasised that a joined-up, system-wide approach is essential for successfully embedding interdisciplinary teamwork (IDT) in rehabilitation settings. This sub theme has been titled the “lone wolf approach” because to the author’s interpretation, the participants were describing people taking an individualistic approach to care that meant principles of IDT working or person-centred care were not really being fulfilled. Siloed disciplinary approaches were criticized for hindering holistic rehabilitation goals and neglecting shared responsibility.
“It feeds into the myth that rehabilitation is therapy, which, you know… I think for me, rehabilitation is about everything you do trying to get back to life, so it’s about us providing that overall experience and opportunities but yet it’s nobody job in a way to do it, so it’s not my job as an SLT necessarily to do… You know, if I was to go into that, and that’s nearly where we’ve gone to. Everybody in a box and a discipline around the individual and that ability to blur and to do shared things. The sharedness of team. That shared tasks of a team, shared responsibility of a team.” Participant 4.
This ties into the identified need for continuous education, and a shared understanding of what “rehabilitation” is. Through reflection, participants emphasized the importance of a collective, “joined-up” approach to creating changes to teams. This includes identifying change leaders and ensuring input from all team members, though this was acknowledged as a challenging process.
“doesn’t matter whether you call it team training, whether you call it person-centred care, you could use any approach going, but you have to have people who say, ‘We’re all doing this and we are going to invest the time, and we’re going to value that, because it will make us more effective in our jobs’. But if you don’t believe that and you believe actually it’s all about the doing, ‘If I do this in my isolation…’ and that’s really important, it’s more important they get my physio than they get this whole teamworking in a more coordinated, a more collaborative manner, then we don’t want to invest and we don’t see it as being valuable.” Participant 2.
The central organising concept for this theme is the participants’ narrative of the default mode of teamworking within the hospital, which poses challenges for IDT. They advocated for challenging and dismantling the nursing and therapy divide, prioritizing person-centredness, continuous education on IDT values and rehabilitation, and fostering a consistent, united effort within the organization to move away from siloed disciplinary approaches.
Theme 3—power and identity: threats to hierarchy and status
Subthemes: Threat to the social group—Disciplines as separate tribes; Threat to the individual—Discipline is tied to Identity and Ego.
The organising concept of this theme is a latent sense of fear, mistrust and defensiveness on behalf of staff towards IDT working. The codes here can be categorised in two interlinked subthemes.
Subtheme: threat to the social group – disciplines as separate tribes
The first subtheme is those pertaining to the social element – where a discipline was conceived of as a tribe separate from others, where loyalty to one’s discipline can often prevail over other obligations.
“I think discipline trumps everything for whatever reason. There’s a multitude of reasons but discipline does… Discipline is where you’re holding your heart and your head.” Participant 4.
Subtheme: threat to the individual – discipline is tied to identity and ego
The second sub-theme describes how this operates on the individual level—that discipline is tied to one’s professional and personal identity. As such, blurring disciplinary boundaries was seen as provocative by many, leading to fear and resistance. This was implicit and explicit in the participants’ accounts -that challenges to the existing siloed approaches were sometimes perceived as threatening to one’s status (“… you want to make everyone a healthcare assistant”) within the existing hierarchy and indeed one’s very worth and value as a healthcare professional. For example:
“As we’ve said, if I give you my superpower, you’re going to ask about the stairs, I will be diminished. I will have lost something of my superpower.” Participant 2.
“We don’t live the practice… I think that we are too precious. We’re so precious that we can’t see that blurring, sharing, is about getting better, not about losing anything. It’s adding things. And that seems to be a real challenge that we cannot crack.” Participant 2.
Participant 1 noted that where the values of person-centred care are truly held, it can act as a sort of antidote to issues of ego “… you should be able to park your ego”.
These subthemes highlight the complexities of professional identity discussed by participants. Another relevant aspect is the notion of being perceived as rehabilitation experts. As Ireland’s only specialist neuro-rehabilitation hospital, staff are inherently viewed as experts in rehabilitation, a fact which can be used to hinder change efforts and maintain the status quo.
“but this is what we do… it’s almost like, again we don’t believe that because this is what we’ve seen and we’re the experts” Participant 2.
Presented here is a pervasive fear and protective element to one’s identity—participants discussed how staff fear undermining their expertise by asking questions or appearing incompetent. The protective factor underlines much of the theme, a defensiveness of one’ professional identity and thus changes—in particular the blurring of disciplinary boundaries can be perceived as a threat to this identity.
This theme intersects with Theme 1, which depicted the ongoing battle for change amid resistance and burnout. The link between these themes highlights a need for control, as staff experiencing change exhaustion may revert to familiar, discipline-specific practices rather than fully embracing interdisciplinary team (IDT) changes. This finding aligns with research on change fatigue, which suggests that change initiators overwhelmed by continuous transitions may become resistant to new initiatives, preferring to rely on established routines as a coping strategy [22]. Ensuring structured support mechanisms, clear communication, and staff engagement in the change process may help mitigate this tendency and facilitate a more sustainable transition to interdisciplinary practice. This is offered by the participants as an explanation for staff resistance to IDT changes below.
Participant 4: I think people are pulled in so many different directions, to be honest. And I do think the kind of, I think it’s natural, the self bit, does you know, kind of my physio, my whatever, my rules is ….
Participant 1: “But there’s no control of that as well, you can control that much more easily … Nearly as you’re getting pulled in all directions, that’s the easiest thing to do, you can timetable, get through the week, get out of here again, because otherwise I’m just going to be ….”
Issues described within this theme relating to power and control permeate the other two previous themes. Where theme one and two describe the nature of the challenges and resistance to changes to healthcare teams as a disruption of the status quo, this theme focuses on the very source of the resistance. For many, IDT working poses a mechanism to dismantling an existing hierarchy among change initiators and their healthcare colleagues and can be interpreted as a threat to one’s current professional standing within that hierarchy. The fear of a loss of power permeates the “battle” described by the participants.
link

