Dental access remains a significant barrier to HNC patients. In addition to this, there is evidence that oral health is a concern for one-quarter of HNC patients after cancer treatment. Some studies suggest that the dentist is the most requested healthcare professional by HNC patients.16
Despite this, there is a lack of evidence investigating the reasons for dental access being such a challenge in HNC patients. There are multiple potential barriers to access, particularly in individuals with a low SES.13,15 An in-depth understanding of these challenges is essential to targeting access programmes.
The potential barriers to dental access for HNC patients are summarised in Figure 3.
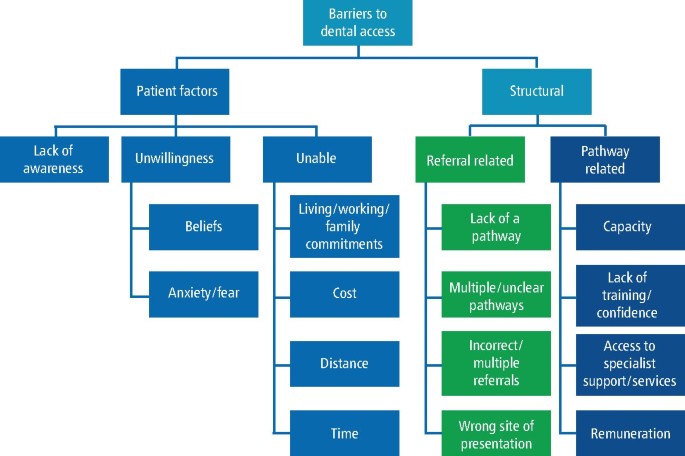
The potential barriers to head and neck cancer patients accessing routine dental care in primary dental services
Developing a safe discharge network (SDN) in West Yorkshire facilitated an improved understanding of the challenges to delivering care for HNC patients through a survey of dental practices in the West Yorkshire Local Dental Network (LDN). Delivery of dental care to HNC patients was discussed at an online practitioner engagement forum. The aim of this workshop was to identify key barriers to the delivery of care. The forum consisted of general dental practitioners during a LDN meeting. Practices were identified by a survey of dental practices in the region, which was led by the LDN chair. The LDN is a local network hosted by NHS England (NHSE), though its future remains unclear since the announcement in March 2025 of the abolition of NHSE. It consists of dental representatives, commissioners, public health officials, patient representatives, and NHS improvement leads. The process in West Yorkshire involved collaborative discussion to identify as many barriers to care as possible.
The survey consisted of four sections:
-
1.
Practitioner information
-
2.
Confidence in providing treatment types in non-case specific scenarios
-
3.
Confidence in providing treatment in case-specific scenarios (five cases)
-
4.
Practitioner support for interventions to improve confidence.
The survey was disseminated to 541 dental practices in Leeds, Yorkshire using a digital format (Microsoft Forms). All data were collected in an anonymous manner; however, respondents were given the opportunity to provide feedback or make queries via email. The contact details of these individuals were kept separate from the survey results, and all data were handled in accordance with information governance policies at Leeds Teaching Hospitals Trust and the Data Protection Act (2018). Individuals were provided with an introduction to the purpose of the survey and an estimate of the time required to complete the survey (11 minutes). Individuals were also provided with a survey completion deadline (30 days).
Data were collated in a Microsoft Excel spreadsheet and analysed using simple descriptive statistics.
Information from this initial phase informed the survey contents. All NHS practitioners registered with the West Yorkshire health service were provided with information on how to access the survey. This was disseminated by the commissioning health service via registered dental practice email addresses in line with accepted information governance principles and consent.
The survey identified three key themes as barriers to the provision of primary dental services for HNC patients:
-
1.
Practitioner training and confidence
-
2.
Remuneration
-
3.
Access to specialist services.
The results of this process as summarised in an earlier publication.17 Further engagement sessions were held between dental practitioners who provided their contact information and the LDN. This discussion process explored methods to overcome barriers to access, while focusing on key aspirational outcomes for patients:
-
1.
Guaranteed dental access at the point of delivery for all cancer patients (irrespective of their pre-existing access to dental services)
-
2.
Guaranteed provision of care as per quality standards (Box 1).
The discussion process led to recruitment of eight dental practices across West Yorkshire in alignment with the above goals. Dental practitioners were supported with the delivery of care by provision of up to four times yearly education sessions on methods of care for, and overcome barriers to care for, HNC patients. Practitioners were also offered streamlined access to specialist advice, guidance and (where required) treatment via a referral pathway to the Leeds Dental Institute.
Following initiation of this pathway, one dental practice has left the network following sale of the practice; however, the network has expanded to include several services within the salaried Community Dental Services. A two-year survey of recruited practices has identified improvements in the proportion of respondents who were confident in the providing care for HNC patients with regard to:
-
Examination and assessment
-
Prevention
-
Stabilisation of caries and periodontal disease, and composite bonding
-
Endodontic treatments (including with inter-incisal opening <30 mm)
-
Provision of fixed and removable prosthodontics.
The confidence of general dental practitioners in providing dental care for HNC patients is summarised in Table 1. In total, 60 individuals responded to the first survey (11% response rate) and 49 individuals responded to the second survey (9% response rate). All questions were answered and completed fully. The survey required a mean time to completion of 9 minutes and 23 seconds.
These data highlight that while remuneration and the number of dental practices may be barriers to dental access, there are numerous other barriers to the provision of dental care that can be overcome through the formation of collaborative networks between primary care and specialist services.
Recent guidance published by NHSE further highlights the role of commissioned pathways to support the care of HNC patients.18 While this guidance documentation highlights the need for specific pathways, and the importance of safeguarding standards of care, it does not specify the structure of services. Indeed, it is likely that models of care will need to remain flexible between regions and over time to ensure that new and persistent barriers to care are addressed through collaborative action. This will be based on a number of factors, including:
-
Pre-existing barriers to dental access
-
The geographic distribution of patients
-
Access to postgraduate-funded education
-
Access to remuneration models (such as flexible commissioning).
link