The survey was made publicly available on January 10th, 2024, and it was closed at the end of February 2024. Within this period, a total of 423 HCPs filled in the survey. The median time for completing the questionnaire was 6.8 min (interquartile range 3.6—13.7 min). The statistics were performed by developing Python and R scripts, that are available on GitHub (https://github.com/bmi-labmedinfo/Fit4MedRob_Surveys/).
Current landscape of robotics rehabilitation in Italy
The pie chart in Fig. 2 shows the percentage of the different professional categories that answered the survey. Most respondents were physiotherapists (almost 45%), while around 15% were physicians. A non-negligible fraction of the respondents were psychologists (12%). Around 9% were Neuro and Psychomotor age therapists, almost 6% were occupational therapists, 3.5% were nurses, 2.4% were educators, and almost 2% Nursing Assistant/ Unlicensed Assistive Personnel. Almost 9% did not precisely indicate their professions. Among the “Other” answers, 78% specified that they are speech therapist.
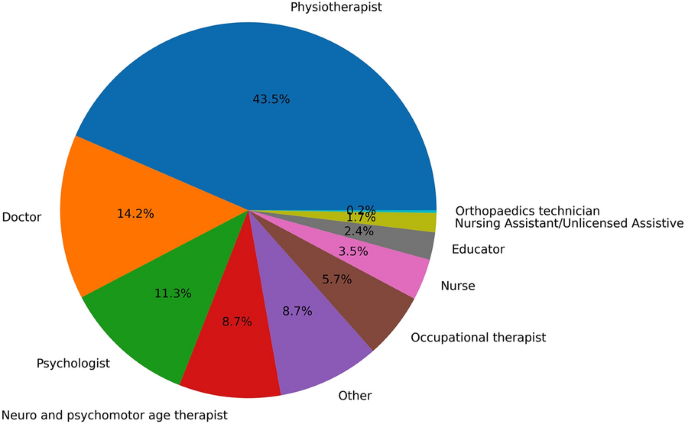
Percentage of respondents for each profession
Regarding the age of the respondents, nearly 23% were between 21 and 30 years old, almost 30% were between 31 and 40, 21% were between 41 and 50, 21% were between 51 and 60 and 5% were above 60 years old. Thus, we have a prevalence of young operators.
As for gender distribution, notably, most of the HCPs were females (73%), 26% were males, and the remaining preferred not to declare.
Considering the physiotherapists, who represent the majority class of our answers, we found that age and gender were distributed very similarly to the reported statistics of the general physiotherapist population in Italy. In particular, the national physiotherapist society (FNOFI, Federazione Nazionale Ordine Fisioterapisti Italiani) reported that in 2023 the percentage of females was 58,9%, and 42,03% of the Italian physiotherapists were under 40 years old [22]. In our sample, we have a proportion of 61% of females, and 43% under 40, which reflects the general population.
We then stratified the respondents across years of experience in rehabilitation (in general), and years of experience in robotic-assisted rehabilitation (Table 1). Among professionals with less than one year of experience in rehabilitation, 82% have no experience with robotic devices. Among participants with 2 to 5 years of experience in rehabilitation, most of them (67%) have no experience with RADTs. Among the 33% of respondents with experience with RATDS, almost 20% of them throughout all their working experience (from 2 to 5 years). Only 10% of the respondents have been working with RADTs since the beginning of their careers.
Figure 3 shows the landscape of the respondents’ settings of work. Among them, 35% work with outpatients, 33% are in post-acute hospital rehabilitation, 6% are in acute care units or research laboratories, and about 5% are involved in home rehabilitation.
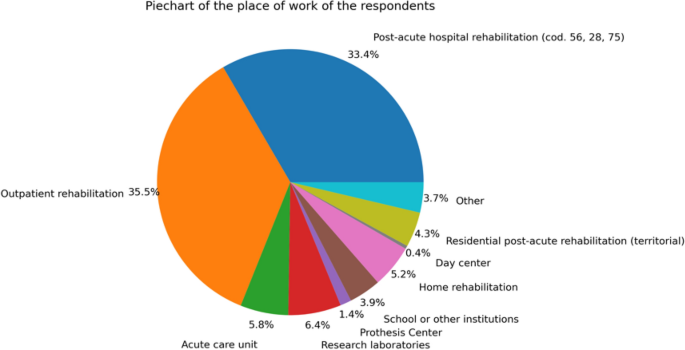
Working settings of the respondents
We then evaluated the clinical experience of the various professional categories in terms of the pathologies of the patients they work/worked with (Fig. 4).
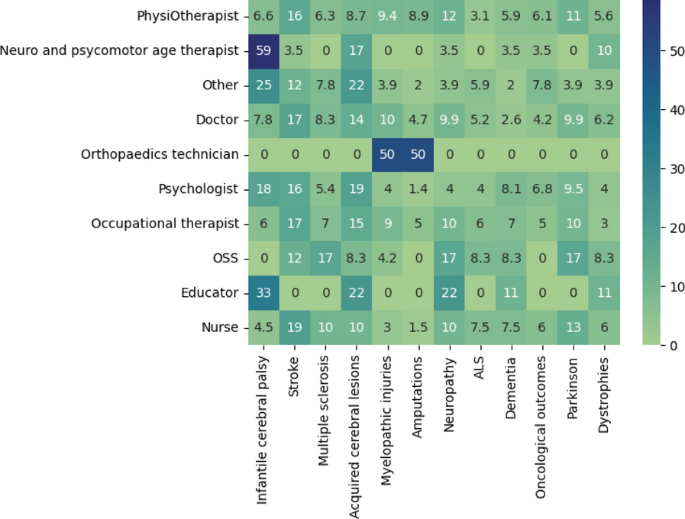
Heatmap showing, for each professional type, the percentage of answers that indicate to work with a specific clinical picture
HCPs attitude towards robotics devices in rehabilitation
Table 2 reports, for each device category, the number of respondents who use devices from that category, the number of respondents who know the devices but never used them, and the number of respondents who are unaware of those devices.
In the following, we report the results of the survey across the 8 different functional device categories, stratifying according to the respondents that use/have used the device or know the devices but never use them. For each question, the answer was given on a 5-level Likert scale (Strongly Disagree, Disagree, I do not know, Agree, Strongly Agree).
For the analysis, we grouped “Strongly disagree” and “disagree” into “I disagree”. The same logic is applied to “Strongly agree” and “Agree”. Specifically, the respondent is asked to answer eight questions (RQ2), related to:
-
Usage of the device: whether they like to use or prescribe the device.
-
Improving the practitioners’ work: whether the device has improved the capabilities of the operators.
-
Improving the patient’s health status: if they believe that the device has the potential to improve patients’ clinical outcomes.
-
Promote participation: whether the device can augment patients’ and/or relatives’ participation in the therapy.
-
Adding value to standard rehabilitation: whether the device can add value in comparison with a traditional rehabilitation.
-
Appropriateness within current clinical practice: whether the usage of a device is appropriate within your current clinical practice.
-
Opinion of colleagues: whether trusted colleagues think that they should use the device.
-
Opinion of supervisors: whether their supervisor believes that they should use the device.
Figure 5 shows the percentage of respondents who agree with a specific statement among those who currently use the device and those who do not use the device but know about it. As expected, most of the respondents who know the devices but do not use them, are not able to express an opinion (Table S2–S9).
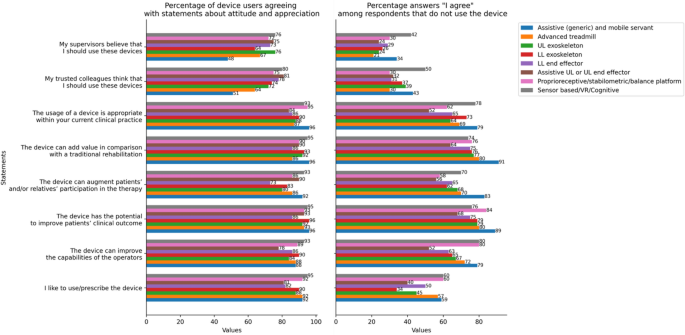
Histogram showing the percentage of device users agreeing with each statement on their attitude and appreciation for the device (left pane) and percentage of answers “I agree” among respondents that do not use the device (right pane)
The proportion of HCPs who express satisfaction with using the devices is consistently high, always exceeding 80% (see Table S2 for specific details). The highest percentage is achieved by sensor based/VR/cognitive systems that reached 95% of satisfaction, while the lowest percentage is related to Assistive UL or UL end effector (81.25). A very few respondents (from 1 to a max of 3) are not satisfied with some devices (Table S2).
Exoskeletons, followed by end effectors, are the devices with the highest percentage of “I do not know” answers.
For the devices users, the majority agree that the device can improve their work capabilites, between 78 to 93%, depending on the type of device (Table S3). Only a few people answered that their capabilities are not improved using the device (1 to 3%). For 3 types of devices (assistive and mobile servant/Proprioceptive-stabilometric-balance platform/Sensor based-VR-Cognitive), the respondents’ opinion of non-users is close to the actual users’ opinion: 80% of them think the use of the devices could improve their capabilities.
Most of the respondents agree that the devices can improve patient’s clinical outcome, whether they use or know the device (from 68 to 96%). Among the users, a maximum of 2 professionals do not agree and a maximum of 4 respondents do not have an opinion (Table S4).
The majority of users agree that each device can promote participation (Table S5). We can notice that for two categories of devices (Advanced treadmill and LL exoskeleton), the number of users that disagree is slightly higher (respectively 6 and 4 persons).
Table S6 shows that, in general, respondents agree that the RADTs can add value in comparison with a traditional rehabilitative approach. For the users, the percentage is always ≥ 86% across the device categories, but also for non-users at least 64% of the answers are positive. Considering the 2 groups of respondents, only a few of them (maximum 6) disagree with the claim.
Across the different types of devices, more than 84% of the users expressed that using robotics is appropriate within their clinical practice (Table S7). Higher negative perception is related to lower limb end effector (13%) and exoskeletons (8–10%).
Regarding the opinion of colleagues, the rate of ‘I don’t know’ answers is important across the devices, also for users (Table S8).
As for the colleagues’ opinions, the rate of uncertainty is high also regarding the opinion of supervisors (Table S9).
We then analyzed the relationship among HCPs subgroups and their attitude toward robotics (RQ4) using a stepwise linear regression. Subgroups have been identified through the profiling attributes indicated in the first section of the survey (inlcuding age, gender, and profession). Table 3 reports, for each device category, the covariates whose estimated coefficient has a p-value < 0.05.
Needs and barriers
The second set of questions is related to the perceived barriers to the spreading of each device category in clinical practice (Table 4).
Lack of financial resources is perceived as a barrier to the usage of all devices in clinical practice, especially for lower limb devices such as exoskeletons and end effectors. On the contrary, the motivation of patients and/or caregivers, as well as the robustness of the device is not seen as an impediment. Lack of training prevents the usage of assistive mobile servants, but it is significant also for other devices. Lack of trust is seen as a barrier by 43% of respondents for LL end effector and by almost 42% for sensor-based, VR and cognitive. For the other devices, lack of trust is seen as an impediment in less than 30%. 32% of participants do not have a clear opinion about the lack of trust in UL exoskeleton.
The scarcity of scientific literature supporting the usage of the device is observed as a barrier across devices, with a higher percentage for assistive and mobile servants. Lack of space is perceived as a strong barrier, especially for lower limb end effectors. Also, time to prepare and re-establish technological stuff before and after the rehabilitation sessions can represent an obstacle to the spreading of the devices, especially for assistive mobile servants. Notably, in this case, no participants declare not to have an opinion. Also, for lower limb end effector all the respondents gave an opinion (either “I agree” or “I do not agree”), but in this case, the proportion of the two answers is similar (52% vs 48%).
Through the analysis of the perceived barriers among participants who do not use the devices but know them, the percentage of answers without a clear opinion (“I do not know”) is not surprisingly higher (Table S10). The results, however, seem to reflect the views of users respondents.
Usability of robotics devices in rehabilitation
Here, we report the SUS results. Low usability might become a barrier. Table 5 reports the number of participants who were confident about the usage of the device and agreed to fill in the SUS, along with the mean and standard deviation of the SUS score. Table 5 reports the detailed answers to each SUS questions for the three categories of devices, i.e. Advanced treadmill, Proprioceptive/stabilometric/balance platform, and Sensor based/VR/Cognitive, for which we collected the higher number of answers in our population (Table 5). The SUS results for the remaining categories are reported in Table S11 and Table S12.
Most respondents indicate that Proprioceptive/stabilometric/balance platforms are easy to use but you need to learn a lot to be able to use them. They are also willing to use these devices frequently (73%). Overall, they feel safe using the devices. A high percentage of respondents (greater than 80%) appreciate Sensor based/VR/Cognitive devices, as they would like to use them frequently, and stated that they are easy to use (Table 6). Proprioceptive and balanced platforms are those with higher mean SUS scores (Table 5, Figure S1), equal to 67.5.
Free text comments
At the end, the questionnaire included a free text field that respondents might use to provide a comment. Even if there could be some bias (often comments are written mostly by people who have a negative feeling), free-text comments may provide details revealing issues that cannot be identified using purely quantitative/multiple choice questions.
Twenty-eight (6.6%) respondents used the free text field at the end of the survey to write a comment. Some of them commented on more than one issue.
Comments have been analyzed through thematic analysis and summarized in the themes “Barrier”, “HCP attitude” and “Needs” (Figure S2). Note that “barriers” was one of the questionnaire sections. This means that some operators, in addition to filling in that section, felt the need to better specify their opinion by exploiting the free text field.
-
Barriers (12 respondents, 43%):
-
Too complicated compared to traditional rehabilitation (e.g., wearing the device);
-
Lack of training (also complained by operators working in robotics-intensive centers);
-
Lack of motivation for therapists (also due to lack of knowledge);
-
Lack of scientific evidence that does not justify the enthusiasm of robotics supporters;
-
Too time-expensive, also due to technical issues, causing discontinuity of usage, so that the therapist cannot achieve good confidence with the device in a reasonable time;
-
Lack of opportunities: distrust in the possibility of using robotics by HCPs operating in peripherical centers (“it’s only for research centers”) (4 respondents, 15%).
-
Poor adaptability to pediatric patients (1 respondent) and to home-care setting (1 respondent).
-
-
HCPs attitude, i.e., how they relate to robotics (12 respondents, 43%)
-
Operators are in favor of robotics only if it is a companion to the traditional rehabilitation, as robotics alone is insufficient;
-
The physiotherapist must be the final decision-maker, to deem if a patient may undergo robotic-assisted rehabilitation, because the health outcome is highly patient-dependent;
-
Fear of being left out “if you don’t use robotics”.
-
-
Needs (14 respondents, 50%)
-
Desire to better know about robotics (5 respondents, 18%), also because, as two respondents said, if the device is not sufficiently known, it is under-used. Operators are conscious of that, which is the cause of frustration.
-
One respondent highlighted the need for better integration into clinical practice
-
Three respondents believe that it is important to tailor the treatment to the specific type of patient.
-
Three respondents made comments related to how they are using the device, for example stating that they are not using the robots at their full potential
-
Usability has also been highlighted by 2 respondents
-
Seven HCPs highlighted the need for learning, also to increase therapists’ motivation.
-
One respondent raised the need for better integration among the different HCPs in the usage of robotics, calling for multidisciplinarity.
-
One respondent reported the need for sustainability
-
link

