Quantitative analysis of PRP service use
Table 1 offers a comprehensive overview of the total number of users by sex from 2015 to 2022. Over this seven-year span, a total of 6680 persons with disabilities received ICRC PRP services, 33.4% of whom were females and 66.6% of whom were males.
A chi-square test revealed a statistically significant male predominance across all age categories (p value = 0.004) (Supplementary file Appendix 2).
Figure 2 provides an overview of the sex distribution trends in accessing PRP services among different nationalities from 2015 to 2020.
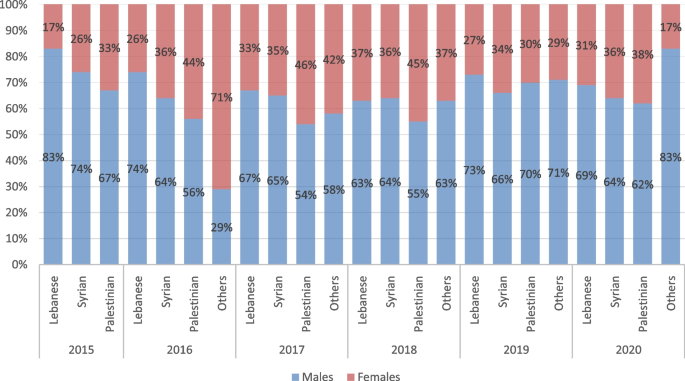
Sex distribution in accessing ICRC PRP services by nationality between 2015 and 2020. NB: Data on nationalities were available for the period from 2015 to 2020
Among all nationalities, a predominant male representation is observed across all age categories, with the notable exception of Palestinian young adults (18–34 y), where the female group constitutes 63% of service users (Table 2).
The main reasons for attending the centers over the study period were amputation (28.1%), cerebral palsy (19.8%), congenital deformity (12.3%), clubfoot (2.1%) and others (37.3%). Figure 4 provides an overview of the amputation-related sex distribution in PRP service access between 2015 and 2022. In the amputee cohort, the sex imbalance was particularly pronounced, with 80.9% being males and 19.1% being females. A chi-square test revealed that among the other physical disability types, men consistently constituted a significantly larger portion, comprising 61.1%, compared to 38.9% women, showcasing a persistent male majority (P-value < 0.001) (Fig. 3).
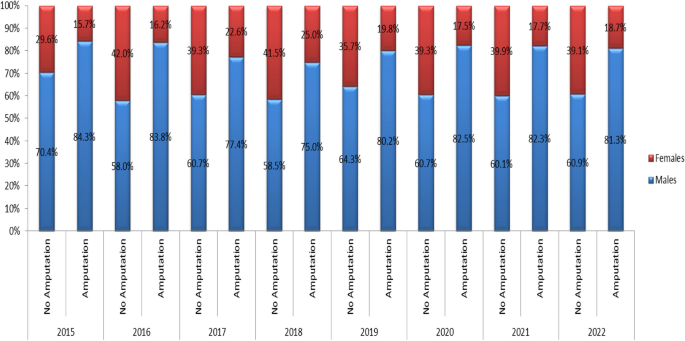
Amputation-related sex distribution in PRP service access between 2015 and 2022
The detailed examination of age and sex distributions among service users attending ICRC-supported rehabilitation centers during the same period revealed patterns that differed between those with amputation and those with other physical disability types. Among amputees, males dominate across all age groups, comprising 80.9%, with the highest prevalence observed in the young child at 91.3% and adult category (18–34 years) at 84.7%. In contrast, females with amputation exhibit a higher representation in the child group (5–17 years) and older adult group ((≥ 60 years) at 28.7%. Among those without amputation, males constitute 61.1%, with the highest representation in the young adult age group (18–34 years), accounting for 73.7%. Females, on the other hand, are more prevalent in the older age categories, with 49.4% in the older adult group aged more than 60 years old (Table 3).
Qualitative exploration of women’s and girls’ health-seeking experience and challenges
Approachability and ability to perceive
Outreach and Information availability
Access to preventative healthcare services, such as vaccinations, was reported by all participants as readily accessible to them, thanks to the outreach efforts conducted by various nongovernmental organizations (NGOs), including the Lebanese Red Cross (LRC), ICRC, and United Nations (UN) agencies. However, information on access to curative primary care at the facility level was reported to be more limited, with several participants indicating that they were unable to find the needed information when necessary. Those who were able to receive information reported receiving information from their family or community networks in the majority of cases or from their physiotherapist in some others.
Fear and health beliefs
Participants emphasized the critical importance of mobility and its prioritization over even basic needs such as food, water, and improved living conditions. This perspective underscores the foundational role of physical mobility in enabling individuals to access resources, maintain independence, and participate in daily activities. In contrast, some participants revealed psychological barriers to engaging with healthcare services. One participant expressed a fear of diagnostic procedures, such as laboratory tests, due to concerns about discovering a potential illness. This hesitancy illustrates the role of health-related anxieties in discouraging individuals from seeking preventive or routine care, even when experiencing symptoms.
Health literacy
Health literacy emerged as a pivotal factor influencing caregivers’ health-seeking behaviors and their ability to navigate the healthcare system effectively. Participants with higher health literacy demonstrated proactive and informed approaches to care. For instance, one caregiver with a professional health background leveraged her knowledge to access preventive and curative services for her children with disabilities, even independently administering over-the-counter supplements to support their recovery. This illustrates how health literacy can empower caregivers to act decisively and effectively in managing their dependents’ health. Conversely, caregivers with limited health literacy expressed confusion and uncertainty about where and how to seek appropriate care, which often hindered timely and effective health-seeking behaviors.
One caregiver, for example, reported:
“Now her Knee Ankle Foot Orthosis (KAFO) is too small for her I don’t know if it is necessary for her to continue to wear them. She used them after her surgery. We haven’t seen a doctor for a very long time.” (P9).
Spirituality
Many participants shared that they have a strong sense of faith even, which helps them be grateful for what they have and believe that a solution will come their way.
“We are relying on God and treating her. Our living situation is like everyone else; we are all living in the same situation in this country.” (P10).
Acceptability and ability to seek
No gender discrimination
No participant, whether a caregiver or girl/woman with disability, reported having been discriminated against on the basis of their gender in healthcare institutions. Some participants even suggested that women might be treated with more respect and compassion than men since they are generally calmer and have a better temper than men.
“No, no, it is all the same. I mean, men were standing waiting just like women, equally. In addition, the treatment, in fact, for men was worse than for women, just so you know. Some of the men were very tense in the health facilities we were in, and there was frustration, irritation, and stress. I mean, you feel that we, as women, have a more positive aspect in that if we are in a certain place, we are treated more politely or better.” (P1).
Societal gender discrimination
As the present study aims to gain an in-depth understanding of the nature and diversity of obstacles experienced by women and girls with physical disabilities to access healthcare services, it was important to capture any social values or gender differences that affected their access. Participants highlighted the intersection of gender and social dependency in caregiving dynamics, emphasizing how societal perceptions and norms disproportionately affect women and girls. A recurring theme was the perception that women are seen as more dependent on assistance but face fewer opportunities to receive it. For instance, caregivers noted that boys often benefit from a wider network of support, with care provided by any family member, whereas girls are typically reliant on female caregivers due to cultural norms.
“A woman is seen as less capable than a man. She is perceived as not knowing as much as a man and as being unable to rely on herself because she has a physical disability. She always needs someone with her, someone to assist her, even for basic needs such as eating. If she were a boy, it would have been easier in all aspects; girls are usually weaker than boys. A girl needs more care. A boy might have his father or brother to help him, but a girl needs her mother or sister for this matter. She requires more attention.” (P12).
“It’s a crime for a woman who has a disability to be uneducated because she will be erased from society; she will never appear to the community; she will be wronged. I see that there are people and families who lack awareness; if they have a daughter with a disability, they hide her from people. She is not seen, no one sees her or knows about her; they are ashamed of her, especially the girls; they do not let anyone see her.” (P18).
Preferences
Participants emphasized the critical importance of privacy and gender sensitivity in healthcare. One participant preferred female healthcare providers for her daughter, reflecting cultural norms that prioritize gender concordance in medical interactions. Another participant recounted her preference for receiving care in a private room to protect her dignity after a visible amputation, underscoring the psychological and social impacts of physical vulnerability.
“She is a girl; it’s good for her to have a female doctor, not a male doctor. Now, my daughter is young, but with older girls, they prefer a female doctor; there should be a choice. Society prefers female doctors more than male doctors.” (P17).
“When I would go to the hospital, I would ask the doctor to provide private room for myself. I did not want to deal with people’s stares or their questions. I would be there for a surgery or a cesarean birth, feeling exhausted, and they would ask why there’s no leg, why a leg is being removed. It is something new to them, the first time they’re seeing such a scene. The questions are very bothersome. I would request to be alone, not wanting anyone else in the room with me.” (P18).
Safety concerns for women with disabilities
One father expressed specific protection concerns for his girl with physical disability, highlighting how this affects girls more than boys. He fears that boys or men might say something to her that is why he feels she needs protection.
“From my point of view, there’s no difference between boys and girls in regard to accessing healthcare services. However, the main issue is that because she is a girl, she requires more attention, and I feel obligated to accompany her to healthcare services. I believe that, as a girl, she is vulnerable and unable to defend herself if needed. I worry that boys or men might say something inappropriate to her, which is why I think she needs protection.” (P13).
Discrimination by nationality
Although all nationalities have been affected by the economic crisis and currency depreciation in Lebanon, Syrians and Palestinians had better access to healthcare than Lebanese because most were already registered in UN & NGOs prior to the crisis and had benefited from NGO programs that target these nationalities specifically. However, two participants suggested that Syrian nationals are more prone to discrimination.
“First, my husband is Syrian, and you’ve seen here the racism in Lebanon and the conditions and circumstances. In addition, the kids they have special needs, and they are two with the same condition that’s why it was hard for us to access healthcare services.” (P1).
Accommodation and ability to reach
Location of healthcare services and transportation
Most participants, independent of their nationality and age, complained that the locations of health care facilities are far from their home, perceiving them as “hard to reach”. Such difficulty was perceived as further exacerbated by the costs of transportation, which led many participants to walk to avoid transportation fees, which in turn exacerbated physical pain and discomfort.
“It is truly far, I am in Akkar and all the physicians and centers I access are in Beirut, I find it difficult to go there because I need to go for several rides, so the main challenge is financial where the ride to reach healthcare facility costs a lot currently” (P10).
“Most important is now the cost of transportation; if I need to go to the center, I need to pay 150,000 LL, so I decided to walk instead of paying for transportation” (P13).
Accommodation
Some participants reported that health care facilities are not accessible for persons with disabilities due to their geographical location and infrastructural barriers.
“I once took her to a center in Khalda where they offered 10 physiotherapy sessions, but she only took 6 because they had stairs and she felt tired of reaching the center” (P8).
Girls are mainly carried by their parents and brothers; in other cases, they may need healthcare assistance, such as ambulances or nurses, while those who cannot find any support report struggling to leave their houses.
She has a front and back walker but is no longer using them, because I am unable to hold her and carry the two walkers; we tried to get out of the house a few times, but she fell and hurt herself. Her father told me not to go out anymore without assistance, and our house is on the fourth floor and there is no elevator.
This barrier is not faced in ICRC-supported facilities, where physical barriers are removed as per organizational standards.
“My mother can move in her wheelchair in the facility to access care.” (p2).
Affordability and the ability to pay
Pay ability
“My husband is an employee in the municipality where they used to cover invoices, tests, and consultations. Honestly these days we are not seeking medical care of any kind even if we need it due to the financial situation, as you know the salary can barely reach 2 million LL… I am aware about the importance of monitoring my health but life hits hard, all we can do is ask about our condition, but we can’t do more” (P6).
“We are waiting for financial assistance to do surgery asap because the treatment has ended… if the money is not collected, 70% we are not going to do it” (P1).
Some participants reported having decreased the frequency of attendance at physiotherapy sessions as a result of their financial hardship.
“I have to do one physiotherapy session per week, but now I am doing it frequently depending on the financial situation, sometimes once every week sometimes once every 6 months” (p5).
Syrians and Palestinians also expressed being confronted with difficult choices when exploring their options to access health care:
“I had to do the hip surgery in Syria and come back because the UN did not cover it” (P10).
Appropriateness and ability to engage
Quality of services
The respondents’ perceptions of the quality of service received varied greatly, with several participants expressing satisfaction with the treatment received and others describing a lack of continuity of care and poor follow-up.
“All I saw were excellent services in the PHCs and at the ones I visit near my house are very organized and have a filing system for everything.” (p11).
“After the KAFO was small, no more services were provided within the organization, so they couldn’t change them. There was no proper continuity in the long term”.
Adequacy of healthcare services
Many interviewees reported that services received at the primary level of care were not sufficiently specialized for their specific needs; in particular, they could not address the rehabilitative care related to their disability.
“I need a specialized doctor in the PHC, I would have access to a family medicine doctor who will provide general prescribed medication, I won’t get proper diagnosis, I want detailed counseling and consultation on all conditions, which is not provided in the PHC” (P14).
Coordination and continuity of the services
Many women reported concerns related to the continuity of services provided at the PHCs. Participants who received their initial devices from ICRC PRP services could not afford to buy new devices when they outgrew them for both women and girls with disabilities; therefore, they have tried to do frequent maintenance rather than replacing the device with a new one as an adaptive mechanism:
“I have been using this prosthesis for 10 years and trying to do frequent maintenance; if it wasn’t for the current financial situation, I would have renewed it” (p5).
A recurrent issue identified was the lack of follow-up from their healthcare providers or the healthcare facilities that they visited, and the absence of feedback mechanisms given to them.
Interpersonal relationships between healthcare providers and patients
Participants’ experiences with healthcare providers revealed a complex interplay between respectful treatment and challenges in communication and system navigation. Many participants described positive interactions, highlighting the importance of being treated with dignity and respect during healthcare encounters. “Nobody treated us badly, nor did anyone uphold our dignity. In contrast, they were very human”. (P1)
However, not all participants shared this positive perspective. Two individuals expressed dissatisfaction with their physicians’ communication, specifically citing a lack of clear and comprehensive explanations about their daughters’ conditions.
“I needed prostheses, so I tried to go to (name of institution), but I did not find any response. Instead, I encountered rude talk and awful behavior. Honestly, I preferred to take a loan and pay for the treatment rather than being humiliated like this.” (P5).
Many participants reported a lack of possibility of directly contacting providers and a lack of coordination among different service providers, which generated difficulties in navigating the system to access the most adequate services.
Policy and legal barriers
Governmental issues
Lebanese participants understood the importance of having a disability card in facilitating their reach to healthcare centers; however, they also acknowledged limitations in the possibilities offered by it due to the financial hardship that national institutions are facing and the inequitable distribution of these disability cards.
“I didn’t get a disability card as no cards are offered now due to the economic crisis, however, sometimes people who don’t need it get it.” (P4).
Unethical behavior remains unpunished
One interesting case involving unethical behavior by a medical doctor was reported by a caregiver for a girl with disabilities. The doctor initially promised medical coverage for the girl but then disappeared, leaving the family in the difficult situation of not knowing how to cover the remaining amount. This disruption severely impacted the girl’s continuity of care, especially since they could no longer contact the doctor for advice on her condition, which required continued monitoring. The family remains uncertain where there are no legal rights to protect them.
Participants’ suggestions
The study participants formulated several suggestions, among which the most recurrent ones were related to the need to integrate affordable and specialized medical services at PHCs, and guarantee financial support and transportation allowances. Other suggestions included improving the availability of information about services available through public channels, establishing local medical centers to reduce transportation barriers, integrating rehabilitative care among primary health care services, removing physical and environmental barriers in healthcare facilities, improving the frequency of monitoring and follow-up for those who use devices over a long time, and planning for continuity of care plans for service users who benefit from devices from initiatives when these services stop.
link

