Participant characteristics
Thirty-seven participants took part in the study. These included 29 nonrehabilitation PCPs, one district hospital manager and seven rehabilitation professionals (six from the district hospital but providing rehabilitation at PHC and one from PHC). Table 1 summarizes their demographic characteristics and duration of experience in PHC.
Of these participants, nine attended the focus groups. The first focus group held in SA consisted of two female PCNs and two female nursing assistants aged between 42 and 58 years with years of PHC experience ranging from 1 to 10 years. The second focus group conducted in Zimbabwe consisted of five female PCNs whose age ranged from 42 to 55 years, while years of PHC experience ranged from 3 to 25 years.
Main findings
The two major themes were described according to the research objectives: (i) the situation of PHC rehabilitation and (ii) the challenges encountered in providing rehabilitation at PHC. The subthemes and categories were derived from an analysis of the participants’ responses. A thematic map of the themes, subthemes and categories is shown in Fig. 2.
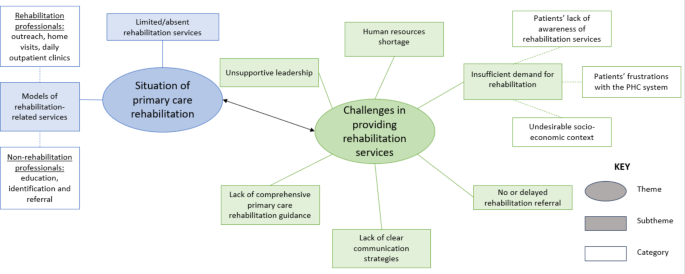
Thematic map of themes related to the study objectives and the subthemes and categories arising from participants’ responses
Situation of PHC rehabilitation
Inadequate/absent rehabilitation services provided by rehabilitation professionals
Although both settings were marked by serious limitations in coverage and capacity, the landscape of health-based rehabilitation services differed between the two countries’ PHC systems. In Zimbabwe, there was a lack of rehabilitation professionals at PHC facilities, with most clinics being operated by nurses without formal credentials in rehabilitation. As one participant said, ‘At the moment, we are only two nurses and one nurse aid’ (P8; PCN; rural; ZW). The situation was the same at the clinics in SA, but some rehabilitation professionals were employed at some of the larger community health centres. One participant listed the professions employed at one facility: ‘We don’t have a psychologist, we don’t have an occupational therapist, we don’t have a social worker…we only have physio, the nurses and the doctors, dental services, and youth’ (P17; PCN; urban; SA).
Models of rehabilitation-related services provided by rehabilitation professionals
In Zimbabwe, outreach services at the PHC facilities, previously provided by RTs from district hospitals, have been discontinued for at least five years. Infrequently, RTs assisted community health nurses when conducting individual home visits in urban areas, but this seemed to be the initiative of the community health nurses, as expressed by one participant who said, ‘the community nurses who do home visits, they are the ones who have to call the rehab and work together’ (FGD 2; PCN; urban; ZW).
South Africa reported a few models of delivering rehabilitation services, but there were notable differences between urban and rural areas. One urban community health centre offered daily outpatient rehabilitation services, but not all rehabilitation disciplines were offered.
‘…so, there’s only one physiotherapist within the facility and no other rehabilitation specialist, and in the case where something is out of my scope when needing other services, I would have to refer to the nearest tertiary hospital…when I’m away there are no physiotherapy services.’ (P16; PHC PT; urban; SA).
In SA’s rural remote areas, rehabilitation professionals were mostly found at district hospitals. These professionals conducted outreach visits and home visits to selected satellite clinics.
‘We also do home visits and then we have one outreach clinic now that we visit once a month… two outreach clinics at the moment per month for our audiologist, she also has an outreach day, so like three clinics basically a month.’ (P22; district hospital OT; rural; SA).
Models of rehabilitation-related services provided by nonrehabilitation professionals
In both countries, the nonrehabilitation PCPs provided patient counselling and education, and referred patients with rehabilitation needs to attend higher-level or private institutions if rehabilitation services were not available at their PHC facilities.
‘We do not provide rehabilitation services, but we refer them to the next level because we’re not like taught on rehabilitation. We can just assist them on how they would go to the [district] hospital and who they are going to meet at the hospital; that is how we are giving help in rehabilitation’ (P7; PCN; rural; ZW).
‘When a patient comes to see a professional nurse, they educate them and tell them to do some exercises at home. For example, we asked them to take a walk. So, they do give them that education.’ (FGD 1; nursing assistant; rural; SA).
‘If the patient is not able to walk, for instance, what we do, we refer so that he can get a wheelchair depending on the disability. We refer because we are a PHC, we don’t have anything here, we just refer, we just refer (clicking)… Even if she is not talking properly, we just refer so that she can meet the speech therapist in [district hospital] ….’ (P12, PCN; urban; SA).
Challenges encountered in providing rehabilitation care at PHC
The various cadres reported several challenges in providing rehabilitation services and ensuring that patients (users) accessed and received quality rehabilitation services. Six themes were identified (Table 2).
Unsupportive leadership affected resource and transport allocation
There was no clear leadership for PHC rehabilitation. This lack of leadership left therapists without the necessary assistive technology and consumables.
‘…the people still in charge are those nurses and maybe those doctors who might not necessarily understand what rehab needs…I think from top down to the actual workers, there’s no input and I think everything is thought of from a perspective of people who have no experience of what is actually happening and so they either have their own perceptions or…little knowledge then we see it kind of spirals down to equipment that’s provided or when it’s not provided and the prioritization of services and finances’ (P16; PHC PT; urban; SA).
Management’s limited understanding of rehabilitation affected human resource allocation, as explained by one participant: ‘There are… healthcare professionals sitting at home waiting to get jobs… for posts where there is a demand, but they are not taking out the money’ (P18; medical officer; urban; SA). The lack of rehabilitation at most PHC facilities precluded many providers from experiencing the benefits of rehabilitation and contributed to their lack of understanding of rehabilitation. One district hospital nursing manager explained, ‘…we don’t think of them sometimes, but if they are near, you can see this thing needs rehabilitation’ (P4; DNO; urban; ZW). Despite the inclusion of rehabilitation budgets at the facility level, the outcomes of these requests were unknown and not followed up. The same district hospital nursing manager admitted that she was ‘not sure about their [rehabilitation budget plan] follow-ups, if what they are getting is enough or are they getting what they have planned but what I know is they are included in the budget’ (P4; DNO; urban; ZW).
Similarly, the lack of prioritization of rehabilitation resulted in transport difficulties for both rehabilitation professionals and patients. In most South African rural settings, rehabilitation services were delivered via outreach from higher levels of care, such as district hospitals. However, the therapists were not supported with transport for conducting regular PHC outreach activities. In some cases, outreach visits to some PHC facilities had to be discontinued due to lack of transportation.
‘Another big obstacle and it comes back to financing, but it also comes back to governance and leadership, is that we really struggle with transport…Often, administration is prioritized; rehab tends to fall pretty low down on the list for transport’ (P22; district hospital OT; rural; SA).
‘We did do outreaches about two or three years ago when I first started working and then there were just a few problems with accessing vehicles and I think it was more institutional problems…’ (P16; PHC PT; urban; SA).
In instances where therapists were able to access transport, the transport was inappropriate for the equipment and consumables needed to deliver appropriate care.
‘There can be some challenges to carrying out services on outreach like, for example, if a patient is needing a wheelchair repair and they took it to the clinic for that day and we didn’t bring every single one of our tools to be able to repair the wheelchair, then there would be a limitation on that front’ (P24; district hospital SLT; rural; SA).
In Zimbabwe, patients were often unable to access rehabilitation at higher levels of care since transport was not provided.
‘…especially if they tell you that they do not have money to go to the hospital. Long back we used to call ambulances…those are the main challenges because we will also not have the means to transport the clients to the hospital’ (P9; PCN; rural; ZW).
Human resource shortages cause work overload and shorter patient consultations
Rehabilitation is delivered in a person-cantered manner and involves individualized assessment and management. The participants revealed that the time available to manage the heavy patient load was insufficient to explore rehabilitation needs. Often, patients and PCPs only explored the main reason for the visit due to time limitations.
‘… you end up not really having enough time with the patient who patient that you can even ask how is home, how are you are staying at home…? You know, you end up just targeting what the patient has presented with… but actually most of their problems may be social problems at home of which we won’t have time to explore every complaint’ (FGD1; PCN; urban; ZW).
The PCPs experienced burnout due to staff shortages. Providers admitted to prioritizing survival over quality of life (which is the crux of rehabilitation) in their management approach to cope with high demands of care.
‘When we are short staffed and there are competing programs, there is a tendency to weigh…which one is more important than the other, looking at which one has the capacity to end someone’s life… looking at survival’ (P8; PCN; rural; ZW).
The effects of staff shortages were also evident in the PHC rehabilitation departments in SA. Patients were often placed on a waiting list and did not receive the prescribed frequency and intensity, affecting rehabilitation quality and outcomes.
‘One of the things that my people have been complaining about…say the dates are very far. You find the person is sick now [June]; he will get a date for next year. So, it is like an insult to them…you will find that they don’t even go when it comes because they have been waiting for so long, so they miss the date’ (P14; PCN; urban; SA).
Lack of clear communication strategies
In most cases, rehabilitation was delivered at higher levels of care (at district hospitals) or – in a few instances – at some larger PHC facilities (community health centres). The PCNs perceived a disconnect between the available rehabilitation professionals and themselves. One participant described how ‘rehabilitation is not something that is very popular like other departments [that] work hand in hand close, close, close… the rehabilitation seems far away’ (P4; DNO; urban; ZW). The poor collaboration resulted in a lack of familiarity and understanding about the roles and contributions of the different rehabilitation disciplines and may have resulted in decreased referral of patients for appropriate care.
In SA’s urban and rural contexts, poor communication also existed between the PCPs and the patients because of varied foreign languages, local languages, and dialects.
‘[T]he language barrier is one of the things that makes difficult to even take history from the client…you have got people from other countries…others are…from the upper parts of South Africa’ (P14; PCN; urban; SA).
‘[T]he majority of our clinical team and the majority of our rehab team are English speakers, and I think 98% of our population in the sub-district are isiXhosa speaking and so that poses a significant barrier to providing quality rehab.’ (P22; OT district hospital OT; rural; SA).
Lack of comprehensive PHC rehabilitation guidelines
The lack of evidence-based guidance compounded by the prevailing siloed university rehabilitation training resulted in fragmented rehabilitation service provision.
‘…the exposure at the varsity [university] level to other rehab professions is quite limited’, making it difficult ‘to understand some of the speech terms or some of [the] management options’ (P22; district hospital OT; rural; SA).
In both countries, the available primary care guidance focused on curative management. Many nonrehabilitation PCPs were familiar with some PHC guidelines, such as the Essential Drug List (EDL), Adult Primary Care (APC) or condition-specific guidelines. However, similar practical rehabilitation guidance was not available; consequently, rehabilitation was often not considered.
‘The [guidelines] are very limited. We have guidelines on the management of hypertensive clients [and] the management of our diabetic clients. But what is lacking is training’ (P8; PCN; rural; ZW).
‘At times you will find that there was no need for medication or a pill but just to tell that person what to do at home… because when you say you’ve got a pain here, what I think is Panado, is Brufen to give you because it’s something that will relieve the pain, there is nothing I would do, say you can exercise and do this, there is no such…’ (P14; PCN; urban; SA).
The PCPs highlighted their adaptability and commitment to lifelong learning if guidelines and training were made available.
‘As nurses, we are very flexible. Like at the clinic, we do most of the work, so if we can do maybe a short course, it would be good for us to help the minor cases, then we refer severe cases’ (FGD1; PCN; urban; ZW).
No or delayed rehabilitation referral
Inadequate referral to rehabilitation was evident in both countries. The absence of rehabilitation services or specific rehabilitation disciplines at PHC constrained PCPs’ capacity to refer rather than indicating a deliberate decision to withhold referrals. PCPs commonly referred patients requiring rehabilitation to doctors at higher levels of care first, potentially lengthening the care pathway for these patients.
‘Since there are not really places where you can refer the clients for speech therapy and all, we don’t usually refer them. We just assist the client in whatever they want, and then they come for their next appointment’ (P13; PCN; urban; SA).
‘We don’t directly refer to them to rehabilitation or even if you see that this condition need rehabilitation. We first refer to a doctor. So, it’s referral to a higher level. Then the higher level will decide if the patient needs rehabilitation.’ (P2; PCN; urban; ZW).
The curative approach to management may explain the delayed referrals as suggested by one participant.
‘[laughter]. For us, pain management is a painkiller. Ya, I’m being honest with you…Then, if that person comes back frequently that is when we would say, this backache I think needs further management’ (P9; PCN; rural; ZW).
Furthermore, some PCPs had insufficient knowledge and awareness of the scope of rehabilitation to adequately identify and refer patients with rehabilitation needs as realized by one participant in SA: ‘I need to look into people who would need it [rehabilitation] even if I don’t think so…and then find out how do we refer and how do we get these services to them’ (P19; PCN; urban; SA). Similarly, the DNO in Zimbabwe observed: ‘There are some gaps because the rehabilitation personnel are the ones who are experts in this area but it’s the nurses who identify and then refer them…They [nurses] don’t have knowledge that would help them to identify the patients and also to help them if they identify a problem who they need to consult’ (P4; DNO, urban, ZW).
The rehabilitation PCPs confirmed the inappropriate rehabilitation referrals, ‘…very often they don’t know what they’re referring for and you will often get someone referring a patient who had a stroke ten years ago… [need to] inform about referral patterns and the referral pathways’ (P16; PHC PT; urban; SA).
Insufficient demand for PHC rehabilitation
The time, resources, and effort spent on conducting outreach visits to the clinics in SA were wasted when few patients attended the scheduled clinics. This resulted in some outreach services being discontinued, as the district rehabilitation professionals decided that they were ‘not really utilizing [their] time very well in going to outreach’ (P24; district hospital SLT; rural; SA).
The participants reported on three factors that hindered patients from seeking rehabilitation in the various contexts:
-
(i)
Patients’ lack of awareness of rehabilitation services
Patients’ lack of awareness about rehabilitation resulted from poor health literacy, cultural beliefs and interrelated myths and misconceptions. Examples of such beliefs were given:
‘If someone has a stroke, they… [think] that the person is bewitched, that is why they are no longer talking or they are no longer walking’ (P7; PCN; rural; ZW).
‘[T]here are a lot of mental healthcare users that don’t present to the hospital or clinic because there’s some entrenched ancestral, witchcraft, traditional ideas about what mental health or mental illness is and what it means and how it’s to be treated…doesn’t quite fit with being treated with western medicine and so the route that patients often take then is in traditional help through a sangoma or traditional medicine’ (P22; district hospital OT; rural; SA).
Thus, in both settings, it was common for patients to seek alternative healthcare from traditional healers or faith healers.
-
(ii)
Patients’ frustrations with the PHC system
Prior negative experiences when attending PHC deterred some patients from seeking further healthcare. One CHW in SA highlighted some healthcare system challenges, including overcrowded clinics and inefficient appointment systems:
‘Sometimes clients block me not to go to their houses. Some are not welcoming at all. Some would tell me straight in the eyes that they are tired of me coming to their houses, telling them to go to the clinic where people must sit the whole day before they can be attended to’ (P26; CHW; rural; SA).
-
(iii)
Undesirable socioeconomic context.
The undesirable socioeconomic context caused patients to prioritize their basic survival over obtaining healthcare and this challenge seemed to be more acute in rural settings. Most individuals in SA’s rural communities depended on social assistance from the government and NGOs for their subsistence, which was insufficient to cover the additional healthcare costs of accessing rehabilitation. To describe the situation, one participant said,
‘Some of them mention that they… do not have anything to eat… Some are not working because they do not even have an ID, but they are in their 30s and 40s… and have no parents… you see the situation is dire’ (P26; CHW; rural; SA).
Poverty in Zimbabwe’s rural communities similarly hindered patients’ access to rehabilitation when referred to higher levels of care.
‘Most of the community, they are peasant farmers and all, so…if you refer them, they talk about the challenge of money’ (P6; PCN; rural; ZW).
Patients may have valued rehabilitation, but financial concerns contributed to patients’ hesitation or inability to seek these services.
link

